Gene therapy is one of the most exciting fields in biotechnology right now, representing a major shift in medicine. It focuses not on treating symptoms of diseases with traditional drugs, but modifying underlying causes in a person’s genetic code.
As a term, you can expect gene therapy to crop up more within the coming years. But what does it actually mean, and what are the ethical questions the come with manipulating people’s genes?
What is gene therapy?
The core of gene therapy is introducing specific genes into a patient to treat disease. Essentially, the aim is to alter a person’s DNA to correct an underlying disorder, such as a mutated gene that may be causing problems with a person’s coding and leading to diseases like cystic fibrosis or muscular dystrophy.
It’s currently an experimental area, but the past year has seen a number of notable advancements. In March 2017, for example, a teenage boy in France was cured of sickle-cell disease thanks to an experimental gene therapy procedure developed by Bluebird Bio.
There are a number of different approaches being tested in gene therapy, which range from replacing mutated genes with healthy copies; to killing off diseased cells; to introducing totally new genes into a body so it can fight diseases.
There are also two classes of gene therapy, dependent on whether the effects are passed on to children or not. Somatic gene therapy involves transferring DNA to cells in the body that don’t produce eggs or sperm, whereas germline gene therapy does involve transferring DNA to these cells. As such, the effects of the former aren’t passed on to subsequent generations, whereas those of the latter are.
How does gene therapy work?
You can’t just inject a gene into a person and be done with it. To get a gene into a cell, it needs to be transported by a special carrier, called a vector. There are several different ways to develop vectors, but one of the main approaches is to use a genetically engineered virus. A category of viruses, known as retroviruses, are very good at introducing genetic material into a host chromosome in order to replicate, and scientists leverage this ability to deliver their specially created gene.
The vector is introduced to specific tissue in a patient’s body, either by injection or intravenously, and then makes its way to the cells. After it has reached the nucleus, it delivers the DNA, integrating it into the cell’s normal genetic process. To treat a disease, this gene will instruct the cell to create a kind of therapeutic protein.
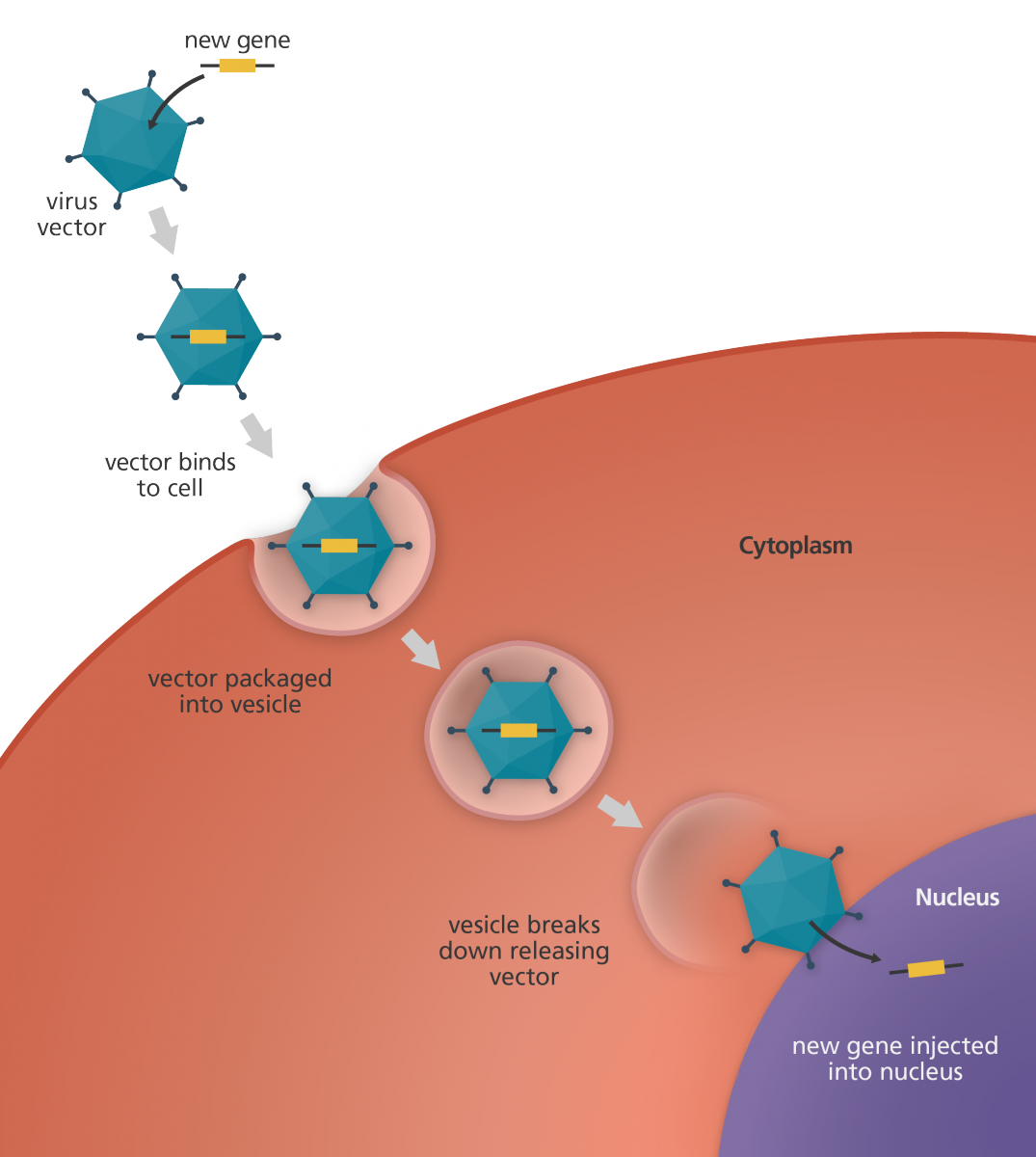
(Credit: Genome Research Limited)
Exactly what that protein does will very much depend on the type of gene therapy being undertaken. It could create a toxic product to kill diseased cells, or it could inhibit faulty genes, or it could add functionality that has been lost due to a disease.
What are the barriers facing gene therapy?
There are really two parts to this: the technical and the ethical.
The technical
From a practical point of view, the most immediate challenge to this process of gene therapy is: a) Making sure the gene reaches the right cells, b) Making sure the gene is actually ‘switched on’. The first needs the vector to be able to target only those cells supposed to be affected by the new genetic code, and the latter relies on the cell not shutting down genes that start performing differently.
Beyond this, the foreign gene also needs to avoid sparking an immune response in the patient. Certain vectors are more likely to be identified as pathogens then others, so the task is to find a carrier that can slip under the immune system’s radar. There’s also the fact that our genetic code is an extremely intricate catalogue of instructions, and if the gene is inserted incorrectly it could ripple out to dangerous side effects. You don’t want to accidentally cause a cancer, for example.
The ethical
From a wider perspective, gene therapy raises a number of ethical questions. When you start editing a body’s genetic code, where do you draw the lines around cells that should and shouldn’t be ‘corrected’? At the moment, research around gene therapy is focused on solving genetic conditions that can’t be cured by other means. In the future, however, as the technique becomes more advanced, what aspects of a person could potentially be changed with gene therapy?
There’s also the contentious question of whether germline gene therapy should be allowed. As mentioned above, this is a type of gene therapy where the effects are passed onto a person’s children. It could stamp out nasty hereditary diseases like Huntington’s, but if done incorrectly it could cause unknown long-term side effects. Even if it works, should we be able to alter genes of those that aren’t yet born?
Regardless of these ethical questions, gene therapy looks to have enormous potential. In tests, gene therapy treatments have restored sight in those losing their vision, and come up with ways to reprogram patient T-cells to sight cancer. It’s very much an area in development, and could cure diseases that were previously thought incurable.
Disclaimer: Some pages on this site may include an affiliate link. This does not effect our editorial in any way.


